INTRODUCTION
The Ortner’s syndrome was first identified by Ortner in 1897 and he described it as the left recurrent laryngeal nerve (RLN) palsy secondary to Mitral stenosis [1]. The primary impact of unilateral RLN palsy is hoarseness of voice which was also reported as the key vocal feature of Ortner’s syndrome. The common pathological cardiovascular conditions which gave rise to Ortner’s syndrome include mitral stenosis, mitral valve prolapse, aortic aneurysm, septal defect, following cardiothoracic surgery, high altitude pulmonary hypertension, ductal aneurysm, and aortic dissection [2,3]. The nature of hoarseness of voice in this syndrome is often inconsistent and reversible. Analysis and intervention of voice in Ortner’s syndrome are utmost important for communication and socio-personal aspects. Satisfactory voice recovery outcomes can be achieved if appropriate conventional and customized voice therapy is provided to these individuals. Even within a short duration, suitable voice therapy can provide evidence-based satisfactory outcomes.
The simultaneous and symmetrical movement of vocal folds facilitates normal voice production [4]. Various intrinsic and extrinsic laryngeal muscles cause movement of the vocal folds which is regulated by the RLN, an inferior motor nerve of the Vagus nerve (i.e., Xth cranial nerve). Any damage to the Vagus nerve or the RLN can lead to vocal fold adductor and abductor muscles denervation, muscle weakness, and vocal cord paralysis. In case of Ortner’s syndrome, the palsy of left RLN restricts medial approximation of left vocal fold causing incomplete or inappropriate closure of the vocal folds [5]. The inability to achieve complete closure followed by partial open phase of vocal folds causes hoarse voice production. Voice is one of the most crucial components of speech, as normal voice production is essential for effective communication. Besides, abnormal voice can also impact the socio-personal, emotional, and overall personality of an individual [6].
In literature, age of identification of Ortner’s syndrome is hugely varying and vocal rehabilitation is rarely documented. Cases of Ortner’s Syndrome have been reported for a wide range of ages, right from one to sixty years with common cardiovascular disorders with comorbid symptoms such as aspiration, pneumonia, fatigue, overall weakness etc. Refer Table 1 [7–20]. Despite these variabilities, voice symptoms are generally consistent, characterized by a hoarseness of voice. Although, acoustic and perceptual assessment of voice quality in Ortner’s Syndrome are commonly performed, voice intervention and voice profiling has been rarely documented. Voice correction in Ortner’s Syndrome must be clinically prioritized after medical intervention as it could facilitate smooth socio-personal rehabilitation.
METHODS
Case report
A 28-year-old woman with a sudden onset of hoarseness of voice due to severe mitral stenosis reported to an Otorhinolaryngologist clinic in Indira Gandhi Medical Hospital, Shimla, Himachal Pradesh, India, a tertiary healthcare center. The manifestation of sudden, non-progressive hoarseness of voice was noticed nearly 8 months before, when she delivered a baby boy. During ENT investigation using fibro-optic laryngoscopy, the patient was diagnosed with unilateral left vocal fold palsy. Further she was referred to a cardiologist for consultation, based on the complaint of breathlessness and fatigue during the day. An echocardiography (ECHO) was suggestive of Rheumatic Heart Disease and Severe Mitral Stenosis along with Aortic regurgitation and Tricuspid regurgitation. Thereafter, she was advised to refrain from any strenuous activity and was put under conservative management. Medicines were prescribed for controlling the cardiovascular symptoms. Further, consultation with a Speech Language Pathologist (SLP) was recommended for detailed voice evaluation before having to undergo any type of surgery. Due consent from the hospital and patient was taken for presenting the case details in an article.
Clinical findings
A detailed case history was obtained by the SLP, which indicated a change in voice in the last 8 months with no other significant medical, familial or physical history. Perceptual analysis of voice was conducted using Consensus of Auditory Perceptual Evaluation of Voice (CAPE–V, ASHA 2003) [21]. All five components of CAPE-V such as roughness, breathiness, strain, pitch and loudness were affected. Pitch and roughness were affected moderately, loudness and breathiness were severely affected, and slight strain in the voice output was also noted. The overall diagnosis of voice as per CAPE-V was moderately-severe hoarse voice. A self-evaluation rating scale, Vocal Handicap Index (VHI-10) was also administered to know the perception of the patient about her own voice and voice symptoms [22]. The VHI-10 consists of 5-point rating scale containing core questions on physical, functional and emotional parameters of the voice. The findings of VHI 10 revealed that the voice quality of the patient was severely abnormal, and it was also impacting her day-to-day life significantly. Besides perceptual assessment, objective voice evaluation of the patient was performed using PRAAT software (64-bit; Windows version, GPLv2–1991, Latest Version 2021), downloaded on a Lenovo G50 Laptop [23]. The patient was seated comfortably at a distance of 6-inch from the microphone and was instructed to phonate the vowels /a/,/i/ a/,/u/ for the maximum duration possible. Recording after every third session i.e., 1st, 3rd, 6th and 9th session were done in a quiet clinical room, under controlled environmental sound condition. Apart from phonation, counting sample from one to ten in Hindi (native language), reading sample of rainbow passage and 1–2 minutes conversation sample were collected. Three samples for each sound were recorded and saved digitally as .wav files. The fundamental frequency (f0), pitch range, intensity, jitter and shimmer, and quality of voice were analyzed and documented. It was observed that the f0, pitch range and intensity were moderately lower than the normal range and jitter and shimmer were severely affected. Based on the perceptual and objective evaluation of voice, the patient was provisionally diagnosed as having moderate hoarse voice. After co-interpreting the subjective and objective voice evaluation outcomes, the vocal rehabilitation program was designed.
Intervention program/Description of treatment approach
A treatment approach was designed following the baseline findings of the acoustic and perceptual parameters of the patient [24,25]. The primary objective of the therapy was to improve vocal fold approximation to counter the impact of left RLN palsy. As hoarseness of voice was the core complaint of the patient, a two-week voice therapy program was designed by incorporating two voice techniques, namely, Push and Pull technique [26] and Head positioning method [27]. Besides these two therapy techniques, Vocal hygiene protocol was also customized and practiced. Based on the severity of the hoarseness, 45 minutes session for four days a week for two weeks were finalized. A trained SLP with experience and expertise in management of voice disorders provided therapy to the patient. The therapy plan was initiated with push and pull technique which was aimed to achieve effective glottal closure to reduce or control hoarseness. The patient was first asked to sit upright in a comfortable chair with handle and press her hands together in front of the body by crisscrossing her palms against each other. The patient was instructed to inhale comfortably and maximally before pushing/pressing her palms against each other and phonate vowel /a/ gently and for comfortable long duration while pushing phase began. Through this technique, the subglottal air pressure was built, aggravated and it was released while phonating the vowel. It was assumed that with increase in subglottal air pressure, vocal fold approximation can be enhanced which can help in minimizing the hoarseness. For pulling technique, the patient was instructed to interlock her fingers and pull across each other or in opposite direction. After completion of comfortable inspiration phase, the patient was directed to phonate /a/ vowel with the onset of the pulling phase. It was assumed that with increased physical effort the adductor laryngeal muscle will induce additional medial movement of the normal or right vocal folds which can facilitate vocal fold approximation. The pushing and pulling technique was recommended to be practiced thrice a day for ten consecutive days. It took two days for effective learning and proper self-execution of this technique. Subsequently, head tilt and positioning approach was demonstrated to the patient. It was presumed that head positioning will facilitate the vocal cord closure by altering the length and tension of the vocal fold muscles. Patient was instructed to sit in a comfortable chair at upright position and inspire comfortably before turning head towards left from midline followed by right, upward and downward. Phonation was loaded while head position was moved from midline to the four quadrants mentioned above. Head position help in repositioning of the vocal folds was aimed at, which may result in improved voice quality or correction of hoarseness of voice. Under vocal hygiene program, the concept of voice misuse, overuse and its impact on voice was explained to the patient. The importance of minimum speech utterances, adequate pitch and loudness level and hydration of vocal folds were advocated and practiced. Besides, the importance of hydration of vocal folds, avoidance of oily and spicy food which may cause laryngeal-esophageal reflux, avoidance of throat clearing and initiation of dry swallow before starting to speak, and not to whisper were counselled.
THERAPEUTIC OUTCOMES
Acoustic outcome
The outcome of measurement of various acoustic parameters were conducted at an interval of three days i.e., 1st, 3rd, 6th and 9th days. A comparison across each measurement indicated that after six sessions of therapy perceptually noticeable improvement in overall voice parameters were reported. It was noted that a significant improvement was seen in pitch, loudness and perturbation measures by the sixth session and a complete reversal of her voice was noted by the ninth-tenth session. Component wise progression of voice is documented below. For each parameter, three recordings were taken and mean values and standard deviation were calculated for the same.
Frequency measures
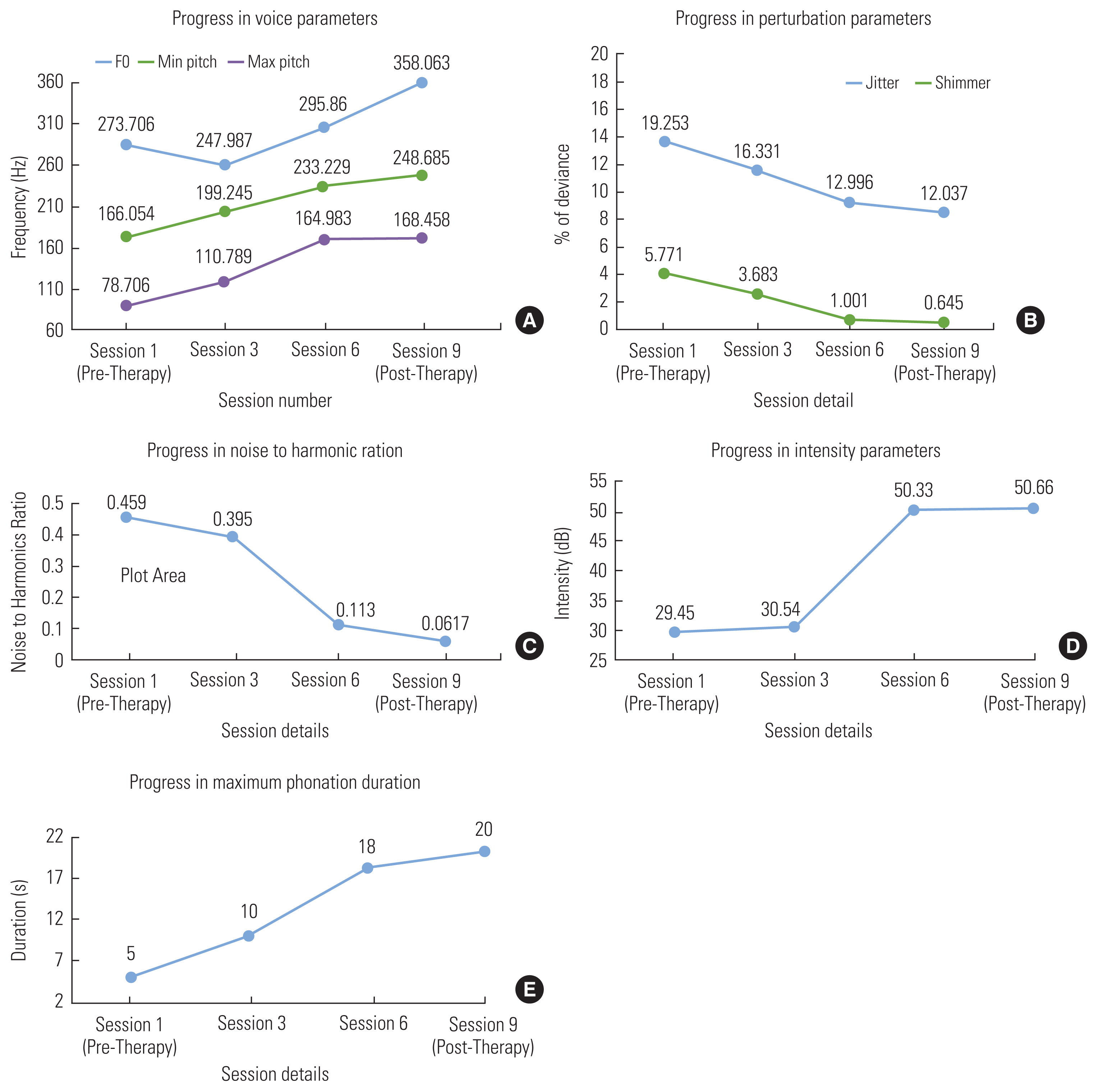
The fundamental frequency, minimum and maximum pitch were analyzed across three session intervals till a total of nine therapy sessions. The mean and standard deviation (SD) of pre therapy f0 was 166.05±3.04 hz which progressed significantly to 233.23±4.26 hz after six sessions and 248.68±3.27hz after nine sessions. Considering the normal f0 range of 190–270 hz [28], it was evident for this patient that her f0 normalized within six sessions of intensive voice therapy. The minimum and maximum f0 were also documented and analyzed. Pre-therapy minimum f0 was 78.71±3.24 hz which improved up to 164.98±3.53hz after six sessions and 168.46±3.07 hz after nine sessions. Similarly, the baseline or pre-therapy maximum f0 was 273.70±3.2 hz which improved to 295.86±3.41 hz after six sessions and 358.06±2.79 hz after nine sessions. Refer Table 2 and Fig. 1A.
Perturbation parameters
The impact of voice therapy on jitter and shimmer were examined and documented. Pre-therapy jitter for the patient was recorded 5.77±1.21 which improved hugely to 1.01±0.36 after six sessions and to 0.65±0.25 hz after nine sessions. Similarly, shimmer was recorded 19.23±1.93 before commencement of therapy which improved to 12.99±2.09 after six sessions and to 12.04±2.02 after nine sessions. Refer Table 3 and Fig. 1B.
Noise and intensity parameters
Noise harmonic ratio (NHR) and mean intensity were also investigated for the patient. Pre-therapy mean NHR was 0.46±0.17 which improved to 0.12±0.12 after six sessions and to 0.06±0.11 after nine sessions. Furthermore, the mean intensity level before introduction of therapy was 29.44±6.53 dB. After six sessions of therapy, it improved to 50.33±4.09 dB, and to 50.66±3.09 dB after nine sessions. Refer Tables 4 and 5 and Fig. 1C and 1D.
Perceptual outcome
The perceptual outcomes using CAPE-V and VHI-10 were measured and a comparison was made between pre-therapy baseline score and post-therapy conditions at an interval of three sessions. The overall CAPE-V improved from pre-therapy score of 74 to 16 by sixth session and zero by ninth session. Similarly, VHI-10 score also improved from pre-therapy score of 68 to 9 by six sessions and 5 by the end of 9th session. Based on the self-evaluation of voice by the patient and the perception of voice by the therapist, the hoarseness of voice of the patient improved from moderate to normal level after six sessions of therapy.
DISCUSSION
Moderate to severe hoarseness of voice was observed in a 28 years old female, who was diagnosed with Ortner’s syndrome, by the ENT doctor after an ECHO. The client was put under medication for managing her cardiac complications and further vocal assessment and intervention was done. Apart from hoarseness, a low pitch, low intensity, high jitter, high shimmer and high HNR were the core features of the patient’s voice. Push and pull technique along with head positioning voice therapy techniques were practiced under supervised condition by the patient. After six sessions of therapy significant improvement across overall voice parameters was observed. Therapy was continued till nine sessions to bring all parameters within normal limits. Post-therapy self-perception, acoustic parameters and as per clinician’s feedback the patient’s hoarseness of voice was regulated.
Though Ortner’s syndrome or cardio-vocal syndrome is a rare entity in clinical practice, consistency of voice impairment specially the hoarseness of voice advocates the vocal rehabilitation of these patients once a patient is medically intervened. Present case study provides sufficient evidence to hypothesize that conventional voice therapy like ‘push and pull’ and head positioning can optimally address the unilateral RLN palsy vocal folds of Ortner’s syndrome. Moderately severe hoarseness of voice was documented in this case study which significantly improved within six therapy sessions. Based on these findings, it could be inferred that the customized therapy approach designed and recommended in this case had higher degree of effectiveness. With reference to the amount of therapeutic gain and recovery of voice within the smallest therapy duration of six sessions, an intervention protocol shall be developed which shall include vocal rehabilitation for every patient of Ortner’s syndrome. Hoarseness of voice shall not be considered as a one-dimensional voice disorder, since it was also affecting day-to-day activity and quality of life of the patient. Vocal rehabilitation can positively magnify the socio-personal interests of the patient as well [29].
Ortner’s syndrome is characterized with cardio-vascular pathology. Cardiac failure, thoracic aorta aneurysm, mitral valve disorders, dilated cardio myopathy are commonly documented which are serious pathologies. Further, there are several comorbid complications associated with Ortner’s syndrome along with core cardio-vascular pathology. Mathai et al. in their case study reported inspiratory strider in a 3 month baby girl with cardiac failure [30]. Madhuraj et al [15]. documented penetration and aspiration along with dysphagia and dyspnea in a 74 years old male patient with Ortner’s syndrome. Thus, primary intervention focus directs on addressal of these complicated cardio-vascular conditions and the comorbid conditions. Often vocal rehabilitation for hoarseness of voice in Ortner’s syndrome are under-diagnosed. Based on the early recovery of voice and the amount of improvement from moderately severe hoarseness to normal voice, as documented in this case study, a modification in intervention protocol for the persons with Ortner’s syndrome is advocated. Awareness about the vocal rehabilitation among the team members dealing with Ortner’s syndrome is required. Literature review on Ortner’s Syndrome suggests that structured and conventional voice therapy is not provided to a huge number of persons with Ortner’s Syndrome who could have optimally benefited with voice therapy.
Findings of this case study explores the role and impact of conventional voice therapy in Ortner’s syndrome. Clinically, outcome of this study will help in understanding the step wise pattern of voice recovery. Evidence based counselling for participation in voice therapy and consistent practice of vocal exercises could be explained using present study. The voice therapy approach customized for this patient in a combination of “pull and push” technique and “head positioning” for three times a day with five repetitions in each practice session yielded significant and rapid voice correction. In future, these treatment protocols shall be further studied on Ortner’s syndrome of varying age range. Voice recovery pattern among Ortner’s Syndrome across various age groups shall be further investigated using either case study or single subject design.
CONCLUSION
A 28-year female reported with moderately severe hoarseness of voice and fatigue while doing routine chores was diagnosed with Ortner’s syndrome. Based on acoustic and perceptual evaluation of voice, vocal rehabilitation program was recommended and practiced. Within six sessions of conventional voice therapy which consisted of pull and push, and head positioning the voice of the patient normalized and by nine sessions voice was generalized specially pitch from 166 to 248 htz. Voice normalization within six sessions advocates the role and impact of voice therapy in Ortner’s syndrome. Findings of this case study suggests that after medical intervention of the Ortner’s Syndrome, voice rehabilitation must be initiated which can facilitate normal voice production.