Kim: Effect of Lexical Retrieval Cascade Treatment on Naming and Discourse of Individuals with Logopenic Variant of Primary Progressive Aphasia (lvPPA)
Abstract
Purpose
The purpose of this study was to examine whether the lexical retrieval cascade treatment was effective in improving single word naming and discourse of two individuals diagnosed with the logopenic variant of Primary Progressive Aphasia (lvPPA) when training was conducted using single word naming and discourse tasks, respectively.
Methods
This study employed a single subject case design. In phase 1, one individual with lvPPA underwent naming treatment to re-learn three sets of words, using semantic, autobiographical, phonological, and orthographic cueing hierarchy. A daily CART-based copying of trained words was given as homework. In Phase 2, the cueing hierarchy was used to improve word retrieval of two individuals with lvPPA in a picture description task. A daily homework of phonological repetitions or orthographic copying was given according to the participant preference. Nicholas and BrookshireŌĆÖs Correct Information Unit (CIU) analysis was used to examine the change in discourse from pre-treatment to post-treatment, and at two-month maintenance.
Results
In phase 1, the participantŌĆÖs naming improved on trained words, however, this did not generalize to the untrained set. Naming accuracy was maintained at or above 60% level, with continued home practice. In phase 2, one participant showed improvement in discourse measures, although the effect size was relatively small. Another participant, who underwent a prolonged hospitalization, did not show improvement in discourse measures.
Conclusions
The lexical retrieval cascade treatment is effective in improving single word naming in lvPPA. The treatment may also improve informativeness and efficiency of discourse when treatment is provided using a discourse level task.
Keywords: Primary progressive aphasia; PPA; lvPPA; Lexical retrieval treatment; Discourse
INTRODUCTION
Primary Progressive Aphasias (PPA) is a neurological condition in which speech and language deteriorate due to atrophy of brain areas supporting communication. In the early phase of the disease, individuals with PPA present with progressive isolated loss of language and speech functions, without significant impairment in other cognitive domains [ 1]. The current classification of PPA involves three variants which are widely accepted by both the research and clinical communities [ 2]. The semantic variant (svPPA), probably the most consistently defined and studied of the three, presents with symptoms caused by widespread semantic system damage, such as loss of word, loss of object knowledge, and surface dyslexia. The nonfluent/agrammatic variant (nfvPPA) typically presents with syntactic impairment in both production and comprehension, as well as speech sound errors reflective of apraxia of speech. The logopenic variant (lvPPA), the most recently identified variant of PPA [ 3], shows the characteristics of impaired naming and repetition, which likely results from a phonological short-term memory deficit [ 2]. These distinguishing clinical characteristics of the three PPA variants reflect the distinctive patterns of brain atrophy associated with each variant [ 2]. In the semantic variant, the atrophy usually involves the anterior temporal lobes (with greater damage on the left), the area critical for semantic memory of objects, words, and facts [ 4]. The most common underlying neuropathology for this variant is FTLD-TDP. In nfvPPA, consistent with the syntactic and motor speech difficulties primarily observed in this variant, the atrophy usually involves the left posterior fronto-insular region. The most frequently reported neuropathology for this variant is FTLD-tau [ 2]. On the other hand, individuals with lvPPA present with atrophy in the left temporo-parietal area, implicated in phonological processing [ 5]. The most common underlying neuropathology for this variant from recent reports is AlzheimerŌĆÖs disease [ 6]. Although the first modern report of PPA cases, by Mesulam, appeared over three decades ago [ 7], research studies investigating intervention outcomes in these individuals have been sparse. The progressive nature of the disorder has likely contributed to this paucity of intervention trials. A recent systematic review [ 8] described a total of 39 behavioral treatment studies published before 2013, many of which reported intervention outcomes involving svPPA. Among the 39, only three articles reported a treatment effect on the more recently defined lvPPA. Including the three new articles published between 2013 and 2016 [ 9ŌĆō 11], this gives a total of six treatment articles involving lvPPA. With the publication of more accurate PPA diagnosis criteria and classification system [ 2], it is expected that there will be more referrals for speech-language therapy for PPA. Therefore, more research is needed to provide treatment options that are effective and practical, especially for less investigated PPA variants. In addition, most of the existing studies only involved only one or two participants, providing a low level of evidence. These single case studies need to be replicated to improve the generalizability of the findings. Not surprisingly, a large proportion of the published invention articles have investigated lexical retrieval treatment for PPA because all three variants show word retrieval difficulty, either prominent symptoms of anomia, as seen in svPPA and lvPPA, or impaired word retrieval in the context of agrammatism, in nfvPPA. According to a recent systematic review on this topic [ 12], behavioral treatment of anomia in PPA is consistently effective in improving the naming of the trained words, however, the pattern of generalization is mixed. Generalization is poor in svPPA whereas individuals with lvPPA often demonstrate generalization to untrained items. However, generalization to a more functional task such as discourse production has been limited in most studies, when the treatment focused on single word naming. While Beeson et al. [ 13] reported significant improvement in speaking rate and efficiency for one participant with lvPPA, other studies [ 9, 14] did not find generalization to discourse production when single word naming was trained. In addition to poor evidence of generalization, single word naming treatment, as has been used in PPA research, is not easily adaptable to a clinical setting. The research laboratory-held treatment sessions are not often restricted by the constraints of a typical clinical setting, such as lack of time for repeated assessments and pre-treatment stimulus selection, limited frequency and length of the treatment, and technology access. Therefore, any treatment, which has shown to be effective in a laboratory setting, needs adjustments so that it could be easily translatable for use in a typical clinical setting.
The present study had several purposes. First, given the paucity of intervention studies involving lvPPA, and the fact that most studies involved only one or two individuals with lvPPA, replication is warranted to strengthen the level of evidence provided by these studies. Therefore, this study employed a cueing hierarchy treatment method reported in earlier studies by Henry and colleagues [ 10, 13] in an attempt to replicate the treatment effect. Second, most of the existing lexical retrieval intervention for PPA employed single word naming treatment. As mentioned earlier, generalization to a more functional task such as discourse production has been limited overall. However, intervention literature of non-progressive aphasia suggests that generalization to discourse is more likely when sentence-level or discourse intervention that targets word retrieval is employed [ 15, 16]. Therefore, this study also aimed to extend the use of the treatment method from its original single word retrieval context to discourse context, in order to examine the generalization effect. In addition, training words selected from naturally occurring instances of word retrieval failure in discourse seems more practical for clinical use. These purposes prompted the following two research questions:
Is Henry and BeesonŌĆÖs Lexical Retrieval Cascade Treatment effective in improving the naming of trained and untrained words in an individual diagnosed with the logopenic variant of PPA? Is the Lexical Retrieval Cascade Treatment effective in improving the discourse ability (as measured by CIU analysis) of two individuals with lvPPA, when treatment is conducted using a discourse-level task?
Based on HenryŌĆÖs findings [ 10], it was expected that the treatment would be effective in improving naming of trained words, following a self-cueing hierarchy intervention using semantic, phonological, orthographic, and autobiographic cues, as well as homework procedures. Generalization to untrained items was also expected. Based on the findings from the non-progressive aphasia literature, it was also expected that the participants will improve their narrative abilities (communicative informativeness and efficiency) if there is not significant cognitive decline during the course of the treatment and between the assessment points.
METHODS
Participants
The data for this study was collected while the participants were enrolled in the Speech and Hearing Center of a University clinic for therapy. Both participants were referred for speech-language therapy from the AlzheimerŌĆÖs Disease and Memory Disorders Center in a large hospital, where they were regularly seen for research and clinical care. Participant 1 was referred first and received single word naming therapy using HenryŌĆÖs Lexical Retrieval Cascade Treatment (ŌĆ£Phase 1ŌĆØ). Participant 2 was referred to our clinic a semester later. Both P1 and P2 participated in the Lexical Retrieval Cascade Treatment at the discourse-level (i.e., picture description) concurrently (ŌĆ£Phase 2ŌĆØ). Assessment and treatment was provided in accordance with the guidelines and semester schedules of the clinic.
Participant 1
Participant 1 (P1) was a 63-year-old left-handed man who reported a 5-year history of word finding difficulties. He received a bachelorŌĆÖs degree and worked as a senior partner at an accounting firm, before he retired due to his difficulty communicating with clients, about a year before he participated in the current study. Since the onset of the problem, P1 experienced depression, anxiety, memory problems involving numbers, and most prominently, word finding difficulties.
P1 was first seen at the AlzheimerŌĆÖs Disease and Memory Disorders Center in a local research hospital for a language and memory evaluation two years prior to his participation in the current study. At that time, neurological and neuropsychological evaluation documented poor paragraph recall (seemingly due to poor encoding), dysfluent speech with word finding difficulties, a dysfluently written sentence, reduced category fluency, and incoordination, demonstrating a pattern of deficits with prominent aphasia suggesting a frontotemporal dementia or AlzheimerŌĆÖs Disease.
At the time of his participation in the study, a speech and language assessment was conducted. The results are shown in Table 1. P1 presented with fluent aphasia and marked word finding difficulties. His narrative on the Western Aphasia Battery-Revised (WAB-R) [ 17] showed use of simple grammatical structures, substitution of a general verb (e.g., do, get) for a specific verb (e.g., getting a fish instead of fishing), empty speech with frequent use of filler words. While his single word auditory comprehension was well preserved, his sentence comprehension was noticeably impaired (34/80 on the WAB Sequential Command subtest). P1ŌĆÖs repetition of words and high probability sentences was preserved, but his repetition of low probability sentences was poor. He named 35 out of 60 words correct on the Boston Naming Test-2 [ 18]. His errors involved 16 circumlocutions with relevant semantic content, 9 phonological paraphasias (e.g., cask for cactus), and 10 semantic pharaphasias (e.g., badger for beaver). P1 showed generally preserved access to the semantic system, scoring 49 out of 52 on the Pyramids and Palm Tree Test [ 19] picture-picture version. In oral reading of a paragraph, P1 misread (e.g., and ŌåÆ has) or omitted words, many of which were function words. In summary, P1ŌĆÖs primary communication deficits were generally consistent with the clinical features of the logopenic variant of PPA. P1 showed the core speech-language characteristics of impaired word retrieval in spontaneous speech and confrontation naming, as well as impaired repetition of sentences and phrases. In addition, three out of four associated characteristics (phonological errors in speech, spared single-word comprehension and object knowledge, spared motor speech production), indicative of logopenic type PPA diagnosis [ 2], were present. This diagnosis was supported by the neuroimaging findings. The SPECT scan report, conducted two years prior to his participation in the study, showed ŌĆ£moderate decreased activity in the bilateral parietal and temporal lobes, left greater than right,ŌĆØ providing support to the clinical diagnosis. As shown on Table 1, P1ŌĆÖs Mini-Mental State Examination (MMSE) [ 20] score was 18 at the time of his pre-treatment evaluation, reflecting the cognitive as well as language deficits corresponding to his five-year history of decline.
Participant 2
Participant 2 was a 74-year old, left-handed man, who reported a two year history of word finding difficulties, which worsened over time. He had masterŌĆÖs degree and worked as a forester at a state agency until he retired six years prior to his participation in the study. P2ŌĆÖs family medical history was significant, in that his father developed early onset AlzheimerŌĆÖs disease with significant language difficulties in his early 40ŌĆÖs.
P2 was first seen at the AlzheimerŌĆÖs Disease and Memory Disorders Center in a local research hospital for language and memory evaluation about a year prior to his participation in the current study. At that time, his neurology exam revealed word finding difficulties with literal paraphasias and memory impairment on both immediate and delayed recall. A subsequent neuropsychological examination, conducted eight months prior to P2ŌĆÖs participation in the current study, showed reduced global cognition (MMSE score of 22/30), impaired executive function, severe impairment of visual organization and cognitive flexibility, impaired confrontation naming, auditory comprehension, and repetition.
At the time of his participation in the present study, a speech and language assessment was conducted. P2 presented with fluent aphasia with word finding difficulties in conversation and naming tasks. His errors on these tasks included circumlocution with relevant semantic content, verbal and phonological paraphasias (e.g., forit for forest), use of simple grammatical structures, and occasional incomplete sentences. Phonemic cues facilitated his word retrieval (correct naming of 38% of the errors on BNT-2). Deficits in auditory comprehension of complex sentences were also noted (64/80 on Sequential Commands subtest of WAB-R), without evidence of agrammatism and spared single-word comprehension.
Although his repetition appeared relatively preserved on WAB-R during this assessment, P2ŌĆÖs primary communication deficits were largely consistent with the features of the logopenic variant of PPA, converging with the diagnosis from his neuropsychology evaluation. His MRI scan obtained a year before his participation revealed moderate cortical atrophy and mild chronic cerebral microvascular disease without hippocampal atrophy. A subsequent PET scan revealed markedly decreased activity in the left parietal lobe and moderately decreased activity in the right parietal lobe, as well as moderately decreased activity in the bilateral temporal lobes, providing support to his clinical diagnosis of the logopenic variant of PPA. P2ŌĆÖs MMSE score was 24 at the time of the language evaluation.
Research design
This study employed a single subject case design.
Treatment
The treatment approach used for both participants was the Lexical Retrieval Cascade Treatment, developed at the University of Arizona and successfully employed with individuals with PPA [ 10, 13]. This treatment was designed to train word retrieval, engaging the residual knowledge in multiple modalities ŌĆō semantic, phonological, and orthographic. In the present study, the procedures were modified to accommodate each participantŌĆÖs cognitive difficulties and preferences. The complete cueing hierarchy used for lexical retrieval training in its original context can be found in Henry et al. [ 10]. As shown in Table 2, the present study used a shortened cueing hierarchy, eliminating the semantic plausibility judgment step, while including questions prompting autobiographical information in the semantic cue category. This treatment method was used in two separate phases of the study. In the first phase, the treatment method was used to train single word retrieval of pre-selected stimuli. Only P1 participated in this treatment phase. In Phase 2, the same treatment method was used to train word retrieval in a discourse context using a picture description task. Both P1 and P2 participated in this phase of the treatment. In both phases, a CART-based homework procedure [ 21] was also used.
Phase 1 stimulus selection and procedures
Stimulus selection
To select the list of training words, 165 words were selected based on P1ŌĆÖs occupation, leisure activities, family structure and activities, household responsibilities, as well as his personal interests. These included 25 action words and 140 object words. Color photographs depicting these words were shown to five healthy individuals (mean age=23 years, mean years of education=17 years, all females) to obtain picture-name agreement data. Words that were correctly named by at least 80% of the pilot participants (130 object and 21 action names) were used to test P1ŌĆÖs naming accuracy. P1 named the 151 stimulus words on three occasions, with a one week break between each trial. Twenty object names were selected as both treatment and generalization probe items largely based on his accuracy level. Eighteen of these words were incorrectly named on all three trials. The other two words (the word suit in Set 1 and spatula in Set 3) were incorrectly named on two out of three trials. The words were divided into four sets of five words, largely matched on the number of syllables and frequency based on MRC Psycholinguistic Database [ 22]. The words could not be matched on familiarity and imageability, because the database had missing values on some of these words. Set 1 words were higher in mean frequency (13.4) than the words in the other three sets, which ranged from 5.4 to 7.4 in mean frequency. The syllable length ranged from 2ŌĆō2.2 syllables across four sets. Each set included mixed categories of words referring to household appliances, clothing items, and vegetables. Therefore, the sets were semantically related to some degree.
Procedures
The words in Set 1 through Set 3 were trained, using a multiple baseline design. The words in Set 4 were used as generalization probe items. The treatment criterion was set at 80% or greater accuracy on a given set across two consecutive sessions. P1ŌĆÖs naming accuracy on all 20 items in the four sets was probed at the beginning of each treatment session, prior to engaging in any treatment activities. Only items named spontaneously or with self-cue (e.g., oral spelling, circumlocution leading to correct naming) were scored as correct. Due to P1ŌĆÖs confusion and difficulty understanding the instructions when multiple pieces of paper were used, the entire cueing hierarchy was organized on a single sheet, and P1ŌĆÖs responses were written on this sheet, including copying of the target words by P1. This helped decrease his confusion. Along with the lexical retrieval cascade treatment, P1 was asked to complete CART-based homework daily [ 21]. He was provided with daily homework packets in which to write the names of the five current target words ten times each, as well as a final recall page to complete by writing the names of the five items in response to corresponding photographs. Two 50-minute treatment sessions were held each week, according to the typical therapy schedule of the Speech and Hearing Center. It took eight sessions for P1 to meet the treatment criteria for the three treatment sets. Naming probe of treatment and generalization targets was conducted immediately after the termination of treatment and at a five month follow-up session, which coincided with the beginning of P1ŌĆÖs clinic therapy the following semester, after the five month-long summer break.
Phase 2 procedures
In Phase 2, lexical retrieval cascade treatment was employed in a discourse context in order to examine generalization of treatment effect to a more functional task. As mentioned earlier, naming treatment involving single word targets shows limited generalization to word retrieval in discourse, the most natural and functional task in which language users engage. In addition, training a participant using pre-selected target words is not feasible in a typical clinical setting, due to the time and effort required to select the words to be trained, and the difficulty of selecting words which are relevant and functional to a specific participant. Therefore, in this phase, the study examined the effect of the treatment when the training was applied to words with which the participant had difficulty naming while engaged in a discourse task. Although the naming accuracy of the ŌĆ£trainedŌĆØ homework words was probed on a regular basis, the effect of the treatment was assessed using narrative tasks administered before and after the treatment.
During this phase, participants were asked to describe photographs displaying typical activities observed in family and community life (e.g., cooking a meal, a family barbeque, grocery shopping, at a checkout counter, at a restaurant). As much as possible, these photos involved scenes which incorporated the personal experiences and interests of the participants (e.g., an Italian restaurant scene, family game night, activity involving a dog). When the participant encountered a word retrieval difficulty, it was determined whether the word was relevant and functional to the participant or not. When it was, the Lexical Retrieval Cascade curing hierarchy was used to help the participant retrieve the target word. Only words deemed to be functional for the participant were used for training, excluding complex or uncommon words that the participant is not likely to use in daily life. At the end of each session, the participant selected the word(s) that he believed to be important for him to be able to remember so that they could be added to his homework list. The homework involved CART-based copying of the target words. This procedure led to a steady increase in the number of the homework words throughout the semester as new word(s) were added each session. The naming accuracy of the trained homework words was probed every two weeks.
Modifications were made to the homework procedures over time. For P1, as the number of homework words to copy increased, the number of copies per each word decreased from ten to five times per word after the first nine sessions. P2 did not want to copy the homework words multiple times, therefore, to facilitate his review of the trained words between two weekly treatment sessions, P2 was instructed to produce the homework words ten times each daily.
Similar to Phase 1, two 50-minute treatment sessions were held each week, according to the typical therapy schedule of the Speech and Hearing Center. P1 and P2 participated in the Lexical Retrieval Cascade Treatment for 40 minutes each session. The remaining 10 minutes were spent on either developing a communication book (P1) or reading Marine-related facts (P2) to accommodate their personal interests.
At the beginning of Phase 2, a few selected measures were administered to P1 in order to document his language and cognitive function at the time he participated in Phase 2 treatment. These measures included MMSE, WAB-R, and BNT. Because P2 only participated in Phase 2, data collected at pre-treatment assessment served as Phase 2 baselines on these formal measures. To examine the treatment effect, four narratives were collected at each assessment point using the BDAE-3 Cookie theft picture [ 23], two pictured scenes, and a picture sequence from Nicholas and Brookshire [ 24]. These narrative tasks were administered at baselines, post-treatment, and two-month maintenance. While two baseline narrative measures were collected from P2, only one baseline narrative measure was collected from P1 due to examiner error. MMSE was administered at pre-treatment and at two-month maintenance (which coincided with the beginning of the following semesterŌĆÖs therapy) but not at post-treatment, in accordance with the procedures of the clinic that all formal assessment be conducted at the beginning of a new semester.
Ethics
The research protocol was approved by the UniversityŌĆÖs Institutional Review Board on Human Subject Protection and monitored by the Compliance Office.
RESULTS
Phase 1
As Figure 1 shows, for all three treatment sets, P1 learned the target words quickly once the treatment began on the set. When he met the criteria of 80% accuracy in naming across two sessions during probe, P1 began the treatment on the subsequent set. Trained set of words was continually probed during the maintenance phase. Set 3 data showed variability in naming accuracy during the baseline phase, suggesting some level of generalization of the treatment effect, however, the trend was not consistently upward. P1 acquired all trained words within 2ŌĆō3 treatment sessions. Naming errors typically involved inability to name or producing semantic paraphasias (e.g., moccasin for slippers). His naming of the untrained words in set 4 did not improve during the extended baselines. Maintenance of all the trained words were high (80ŌĆō100%). Five month follow-up data showed that although P1ŌĆÖs naming of the trained words decreased from the scores at the last maintenance probe, it remained more accurate than at baselines with all three sets at or above 60%. Effect size for the three sets of trained words was calculated using the CohenŌĆÖs d statistic recommended by Beeson and Robey [ 25]. For Set 1, due to the same value of the two baseline measures, the standard deviation ( SD) could not be obtained. Therefore, The SD for Set 1 was replaced by the SD of Set 2 based on one of the alternative methods recommended by Beeson and Robey. As shown in Figure 1, for all three sets of trained words, effect size was above the benchmark set for treatment study of aphasic language deficits by Beeson and Robey (small-, medium-, and large-sized effects corresponding to 2.6, 3.9, and 5.8). P1ŌĆÖs global cognition as measured by MMSE did not change significantly from pre-treatment (18/30) to post-treatment (19/30) to five month follow-up (17/30).
Phase 2
Participant 1
Before P1ŌĆÖs participation in the Phase 2 treatment began, selected measures were re-administered to examine the change in his language and cognitive function between Phase 1 and Phase 2 treatment initiation, which was separated by seven months. P1ŌĆÖs MMSE was comparable between the two phases (18/30 and 17/30, respectively). On the other hand, his language scores had decreased on WAB-R (AQ=70.4 ŌåÆ 64.6) and BNT (35/60 ŌåÆ 20/60).
P1 became quickly accustomed to his new treatment protocol of describing pictured scenes and selecting his homework words at the end of the session. Table 3 shows the increase in P1ŌĆÖs size of homework vocabulary over time and the accuracy on the naming probes administered bi-weekly. After the second probe, P1 experienced a set back resulting from prolonged hospitalization following his abdominal surgery for hernia and blood clot removal. Despite his irregular attendance, the narrative data, the main measure for this phase, were collected as scheduled and analyzed using Nicholas and BrookshireŌĆÖs CIU analysis. P1 showed no improvement in all measures of CIUs from the pre- to post-treatment. As shown on Table 4, the effect size comparing the pre- and post-treatment narrative measures as well as pre-treatment and two-month maintenance measures was negligible, and in some cases showed negative values. During this phase, P1ŌĆÖs MMSE scores changed from pre- (17/30) to post-treatment (10/30) to two-month maintenance (15/30). P1 attended a total of 11 fifty-minute treatment sessions during this phase.
Participant 2
P2 attended a total of 15 fifty-minute treatment sessions without interruption. As shown in Table 3, P2 added new words to his homework word list steadily over time. He was able to name his homework words with over 90% accuracy across all the probe sessions, although the number of words in his homework list increased from 10 words at probe 1 to 31 words by the post-treatment probe. His accuracy of naming decreased to 70.9% at the two-month follow-up, although he reportedly reviewed the words occasionally during the break. P2ŌĆÖs narrative data were analyzed using Nicholas and BrookshireŌĆÖs CIU analysis. P2 showed improvement on all four measures of CIUs from pre- to post-treatment. %CIU improvement was also shown when follow-up measure was compared to the pre-treatment data. However, as shown in Table 5, effect size for all variables did not reach the small effect size benchmark (2.6) set by Beeson and Robey [ 25]. P2 lost some of these gains at two month follow-up. The grammaticality of P2ŌĆÖs narratives was also analyzed using the Quantitative Production Analysis (QPA) [ 26]. The results showed that the mean number of well-formed sentences had significantly increased in his post-treatment narratives ( M=9) as compared to his pre-treatment narratives ( M=4.6; (t(2)=ŌłÆ5.892, p=0.028), along with the increased number of verb tokens from an average of 8.8 (13.4 when including be verbs) to 13 (19.3 when be verbs are included). During this phase, P2ŌĆÖs MMSE scores changed from 24/30 at pre-treatment to 16/30 at the two-months follow-up (which coincided with the beginning of the following semesterŌĆÖs therapy). His BNT score also decreased from 24/60 pre-treatment to 16/60 at two-month follow-up. These external measures were not administered at post-treatment per our clinic policy.
DISCUSSION
The main purpose of the study was to examine whether Lexical Retrieval Cascade Treatment is effective in improving single word retrieval of an individual with lvPPA and whether the treatment method could be adapted to improve discourse in PPA. Our data, combined across the two phases and two participants, provide positive answers to these two research questions with some caveats.
Treatment effect on single word retrieval (Phase 1)
The Phase 1 data from P1 clearly demonstrate that the treatment method is effective in improving naming of trained words in an individual with the logopenic variant of PPA. This finding converges with those of Henry et al. [ 10], further supporting the conclusion that individuals with PPA can improve their naming ability for trained words, when the treatment method and delivery is appropriate for their cognitive and linguistic ability. This finding is very encouraging since, while the typical time post-onset is about two years in many previous PPA word retrieval treatment studies [ 12], P1 was five-years post-onset at the time he participated in the study. In terms of generalization to untrained words, unlike the findings of Henry et al. [ 10] and 6 out of 17 previous studies reviewed in Beales et al. [ 14], P1ŌĆÖs performance on the untrained set did not improve throughout the extended baselines. There are several possibilities for this lack of within-level generalization. First, as reported by Beales et al. [ 14], 11 out of 17 previous studies did not demonstrate generalization. Perhaps generalization is not guaranteed in a progressive disorder, especially when the participant is five years post-onset. Second, while our sets were matched on some variables (e.g., frequency, syllable length, semantic category), they were not matched on some other variables (e.g., familiarity, imageability), and each set was composed of items from three different semantic categories. This means they may not have been optimally constructed to observe a generalization effect to semantically related untrained items. In terms of maintenance of the treatment gains, P1 maintained his treatment gains at or above 60% at five-month follow-up. This finding is similar to the previous studies, which specifically used the Lexical Retrieval Cascade Treatment [ 10, 13], although maintenance of treatment gains has been mixed among previous studies in general [ 12]. However, unlike the nature of the maintenance data in most previous studies (i.e., unpracticed), in the present study, P1 chose to work on his maintenance of treatment gains during the interval between the post-treatment and maintenance testing. Being acutely aware of his deteriorating communication abilities, P1 requested CART review sheets that he could use during the summer break and was supplied with them. He reported to have copied his treatment words daily for the most part of his summer break. Given his decline on other language measures such as WAB-R and BNT-2 during the interval, it is likely that his daily copying of the words using the CART procedure significantly influenced his maintenance result.
Treatment effect on discourse
Lexical Retrieval Cascade Treatment provided using a discourse-level task improved the narrative measures of P2 (although the effect size was small) but not P1. In light of the different outcomes, some of the factors that might have influenced the outcome differently between the two participants were considered.
Participant 1
P1 had participated in Phase 1 treatment and showed improved naming of trained words using the cueing hierarchy. However, he did not show improvement in his narratives when the same treatment was applied using a discourse-level task. While it could be that the Lexical Retrieval Cascade Treatment is simply not effective in improving narrative production in PPA, there also are several factors that might have hindered the effect of the treatment on P1ŌĆÖs discourse-level language use.
First, his overall language abilities appear to have worsened since his participation in Phase 1. Although P1ŌĆÖs MMSE scores did not alter between phase 1 and phase 2 treatment initiations, his language scores decreased noticeably on WAB-R and BNT-2. His response to BNT-2 items suggested further degradation of his phonological knowledge from Phase 1. For instance, his naming of scissors changed from a correct response to sivers. In addition, phonemic cue was less effective, decreasing from 65% effective at retrieving the target word at the beginning of Phase 1 to 25% effective at the Phase 2 baseline measures. For instance, following the phonemic cue for asparagus, which he named correctly in Phase 1, P1 produced spa. Such deterioration, inevitable in a progressive disorder, poorly equipped him for complex language tasks.
Second, P1ŌĆÖs weakened ability to benefit from the treatment was likely compounded by the disruption caused by his surgery. P1 had a one-month lapse in his treatment participation due to his abdominal surgery and subsequent complications after probe 2. The MMSE administered a week before his post-treatment testing, to assess his cognitive status following hospitalization, showed a significant drop in his scores (from 17/30 pre-treatment to 10/30). Therefore, his post-treatment assessment results may not accurately reflect the true outcome of the treatment, but rather, it might reflect the impact of cognitive decline on language function, especially on complex language function such as discourse. At two-month follow-up, P1ŌĆÖs cognitive scores and homework probe word naming had recovered to a great extent, however, his discourse ability as well as his cognitive ability to navigate his environment (e.g., driving himself, finding a place, organizing his daily activities) was irreversibly impaired.
Finally, although not formally assessed, P1 started to show a greater difficulty retrieving verbs than other class words during therapy in Phase 2. Accordingly, some of his CART homework words were verbs that he selected. However, he had significant difficulty naming verbs on his biweekly probes. In discourse, such verb retrieval difficulty hinders forward progression of the narrative, as verbs tend to occur early in sentences, thereby, leading to production of fillers, repetitions, revisions, and overall unproductive narrative.
On the positive side, P1ŌĆÖs Phase 2 data appear to illustrate the importance of ŌĆ£tapping into the residual systemŌĆØ to critically support maintenance of skills in PPA, as discussed by Beales [ 14] and others [ 27]. In phase 2, homework word naming data were not used as a measure of treatment effect because these words were not selected based on multiple naming trials, and therefore, their baseline naming accuracy was not known. However, in light of his worsening access to phonology of the words, his relearning and maintenance of trained words is positive, regardless. It appears that this learning effect is related to his CART-homework procedure to some degree. Although even simple copying was a challenge to P1 by this point, he painstakingly completed his homework, stating that his homework helped him talk better. During this phase, when P1 could not retrieve the name of the trained items on his probes, he sometimes orally spelled part or all of the word (e.g., orally spelling M-U--F-F-L-E-R after incorrectly attempting to produce the word as muddle). While oral spelling often did not lead to the correct verbal production of the target word, correct or even partially correct oral spelling is as effective as verbal production of the word in conveying the message. Thus, P1ŌĆÖs CART homework results suggest that orthographic training facilitates lexical access through an alternative route in the face of deteriorating phonological knowledge in this variant of PPA.
Participant 2
P2ŌĆÖs narrative data showed improvement from pre- to post-treatment in almost all measures of CIUs that we analyzed. However, the effect size of all variables did not reach the small effect size benchmark (2.6) set by Beeson and Robey [ 25]. The proposed effect size values of Beeson and Robey were derived from the meta-analysis of aphasia treatment studies. While the language abilities of individuals with aphasia tend to improve over time, the language and cognitive abilities of individuals with PPA deteriorate over time. In light of this different trajectory in their language abilities over time, the magnitude of P2ŌĆÖs effect size on the narrative measures (the strongest one was % CIU effect size of 2.11) might nevertheless demonstrate positive treatment outcome. Not only his post-treatment narratives included more CIUs, his sentences were more grammatical as compared to his pre-treatment narratives. Although his two month follow-up CIU measures have decreased from his post-treatment measures, his %CIU and CIU/minute measures were still higher than those from the pre-treatment assessment despite the noticeable decrease in his MMSE scores (from 24/30 pre-treatment to 16/30 at the follow-up). P2ŌĆÖs cueing hierarchy treatment was also accompanied by daily homework, however, it was modified to repeating the target name ten times each instead of copying them. It is speculated that, in the early stage of lvPPA, homework involving phonological repetition alone, without orthographic training, is effective in improving verbal naming of trained words, as his homework probe data suggest.
Limitations
The study had several limitations. First, each phase had only one participant who contributed meaningful data. While the first phase accomplished the studyŌĆÖs aim to replicate the findings of Henry et al. [ 10], strengthening the generalizability of the findings from these studies to some degree, the results of the second phase provide weak evidence for the treatment effect at this time, because it essentially relies on data from one participant. Second, due to the constraints on assessment time, the assessment between each phase of the treatment during Phase 2 treatment involved some selected measures in selected intervals only. More frequent and/or comprehensive assessment between phases might have provided further information on the time course of the treatment effect as well as cognitive change. Third, as mentioned earlier, stimuli used in phase 1 were not matched on some linguistic variables, potentially influencing the generalization pattern of the treatment. Finally, both participants are diagnosed with the logopenic variant of PPA, therefore, the treatment effect might only be expected in the same variant of PPA participants.
CONCLUSIONS
This study examined the effect of the lexical retrieval cascade treatment on word retrieval of individuals with the logopenic variant of PPA in both single word retrieval and discourse tasks. The study was conducted in a semi-clinical setting (a university clinic) with the intention of applying research-based treatment methods to routine care of individuals referred for therapy. In this sense, the data from this study could be considered practice-based evidence collected in a clinical setting. The results of the study suggest the following conclusions. First, Lexical Retrieval Cascade treatment is effective in improving single word naming in lvPPA, even in those several years post-onset. Second, the treatment method could be successfully applied to a discourse level task in the early stage of lvPPA, improving informativeness and efficiency of communication. This is desirable because discourse treatment is more functional, practical, and can easily incorporate the participantŌĆÖs preference (e.g., topic and homework word selection). Third, homework-based orthographic training is likely to be beneficial in improving and maintaining word retrieval in lv PPA as it engages the residual system that can support lexical access over time.
As the healthcare community becomes more actively involved in the care of individuals with communication deficits resulting from neurodegenerative disease, more evidence on the efficacy of discourse level treatment methods is necessary. Given its easy implementation in clinical settings, further investigation of the Lexical Retrieval Cascade treatment in individuals with PPA is warranted.
ACKNOWLEDGMENTS
The author thanks P1, P2, and their families for participating in the study. The author also thanks Andrea Marr and Meryl Hoffman for their help in collecting the data for this study.
Figure┬Ā1
P1ŌĆÖs naming accuracy of trained and control words across baseline, treatment, maintenance, and 5-month follow-up. 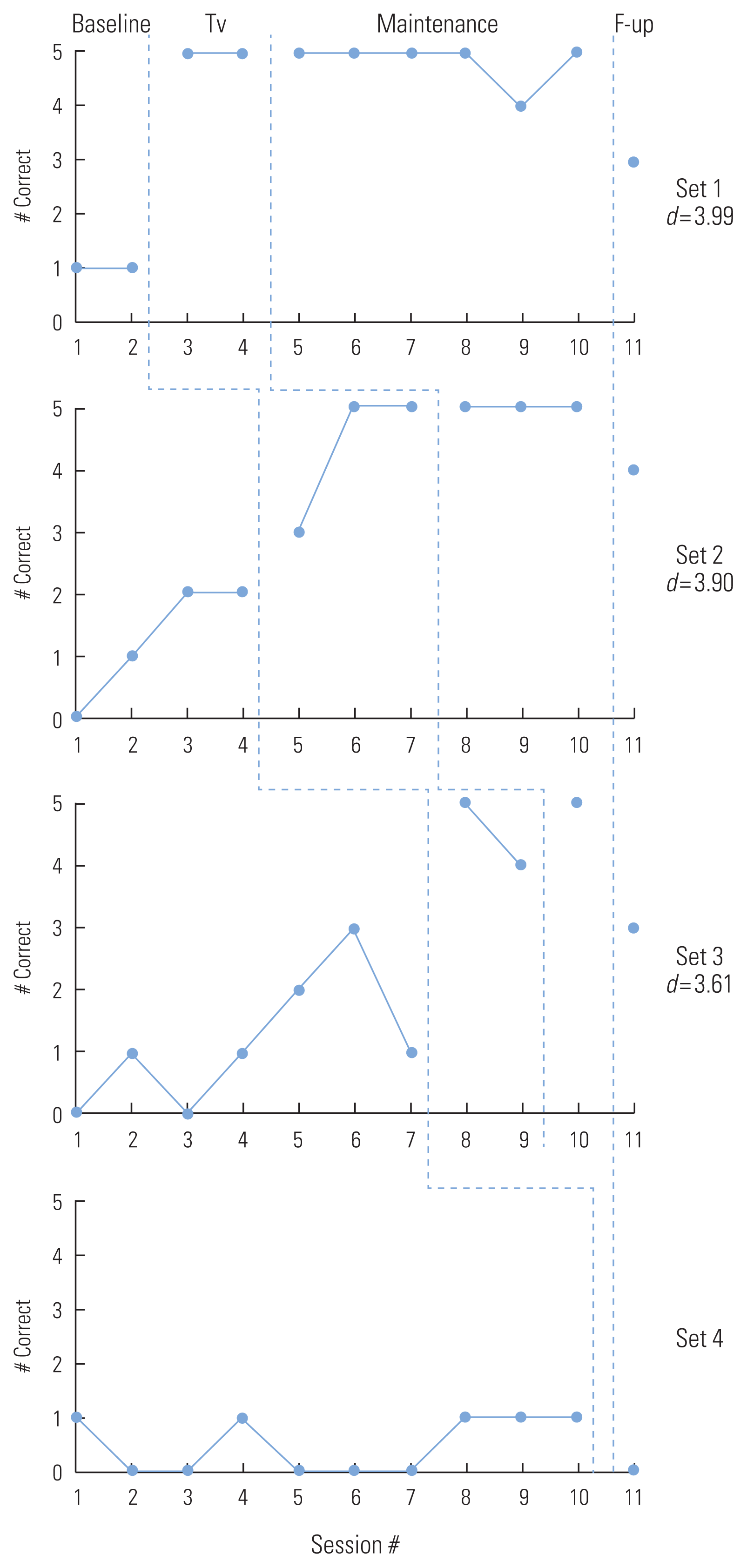
Table┬Ā1
Demographic data and pre-treatment performance of two participants with logopenic variant of PPA on selected tests and subtests
|
Demographic information and test results |
P1 |
P2 |
|
Age |
63 |
74 |
|
|
Education |
16 |
18 |
|
|
MMSE (30) |
18 |
24 |
|
|
Western Aphasia Battery aphasia quotient (100) |
70.4 |
80.8 |
|
ŌĆāInformation content (10) |
8 |
9 |
|
ŌĆāFluency (10) |
6 |
5 |
|
ŌĆāComprehension (10) |
7.5 |
8.9 |
|
ŌĆāRepetition (10) |
7.2 |
9.4 |
|
ŌĆāNaming (10) |
6.5 |
8.1 |
|
|
Boston Naming Test (60) |
35 |
24 |
|
|
Pyramids and palm tree ŌĆōpicture (52) |
49 |
50 |
|
|
PALPA auditory digit repetition span |
3ŌĆō4 |
5 |
Table┬Ā2
Modified Lexical Retrieval Cascade cueing hierarchy used in the study
|
Cueing hierarchy |
Present a picture for naming |
|
1. Semantic self-cue |
Prompt semantic description with, ŌĆ£Tell me about itŌĆØ
Additional prompt examples: ŌĆ£What does it look like?ŌĆØ, ŌĆ£Where can you find it?ŌĆØ, What do you use it for?ŌĆØ ŌĆ£What does it make you think of?ŌĆØ ŌĆ£Have you seen/used/eaten it before?ŌĆØ If unable to provide an answer independently, provide an answer, write it down, and request repetition of the answer
|
|
2. Orthographic self-cue |
Request written production of target word
If unable to write the word, prompt, ŌĆ£Can you write the first letter or any part of the word?ŌĆØ If unable to generate any orthography, clinician provides first grapheme.
|
|
3. Phonemic self-cue |
Pointing to the first grapheme, prompt for the first sound |
|
4. Oral reading |
If unable to independently produce spoken name or written word, clinician adds more letters progressively, until the entire name is written
Prompt oral reading, ŌĆ£What does this say?ŌĆØ Request multiple copies of the written word (3 times maximum)
|
|
5. Repetition |
When necessary, provide the spoken model of the name.
|
|
6. Recall |
Ask for recall of two semantic features and spoken/written name
|
Table┬Ā3
Phase 2 biweekly word probe data for P1 and P2
|
Probe Session |
P1 |
P2 |
|
1 |
83.3% (10/12) |
100% (10/10) |
|
2 |
89.4% (17/19) |
100% (17/17) |
|
3 |
76.2% (16/21) |
91.3% (21/23) |
|
4 |
90.5% (19/21) |
90.3% (28/31) |
|
2 month follow-up |
95.2% (20/21) |
70.9% (22/31) |
Table┬Ā4
Effect size (d) for P1ŌĆÖs CIU analysis results
|
CIU measure |
Post-tx |
2 month follow-up |
|
# words |
0.81 |
ŌłÆ1.43 |
|
# CIU |
0.44 |
ŌłÆ0.11 |
|
% CIU |
ŌłÆ0.28 |
ŌłÆ1.07 |
|
CIU/Minute |
ŌłÆ0.69 |
ŌłÆ1.43 |
Table┬Ā5
Effect size (d) for P2ŌĆÖs CIU analysis results
|
CIU measure |
Post-tx |
2 month follow-up |
|
# words |
0.78 |
ŌłÆ0.24 |
|
# CIU |
1.42 |
0.17 |
|
% CIU |
2.11 |
1.77 |
|
CIU/Minute |
1.64 |
0.74 |
REFERENCES
1. Mesulam MM. Primary progressive aphasia. Ann Neurol. 2001;49:425ŌĆō432.   4. Patterson K, Nestor P, Rogers T. Where do you know what you know? The representation of semantic knowledge in the human brain. Nat Rev Neurosci. 2007;8:976ŌĆō987.   7. Mesulam MM. Slowly progressive aphasia without generalized dementia. Ann Neurol. 1982;11:592ŌĆō598.   9. Croot K, Taylor C, Abel S, Jones K, Krein L, Hameister I, et al. Measuring gains in connected speech following treatment for word retrieval: a study with two participants with primary progressive aphasia. Aphasiology. 2015;29(11):1265ŌĆō1288.  12. Jokel R, Graham N, Rochon E, Leonard C. Word retrieval therapies in primary progressive aphasia. Aphasiology. 2014;28(8ŌĆō9):1038ŌĆō1068.  14. Beales A, Cartwright J, Whitworth A, Panegyres PK. Exploring generalization process following lexical retrieval intervention in primary progressive aphasia. Int J Speech Lang Pathol. 2016;18(3):299ŌĆō314.   15. Antonucci SM. Use of semantic feature analysis in group aphasia treatment. Aphasiology. 2009;23(7ŌĆō9):854ŌĆō866.  16. Falconer C, Antonucci SM. Use of semantic feature analysis in group discourse treatment for aphasia: Extension and expansion. Aphasiology. 2012;26(1):64ŌĆō82.  17. Kertesz A. Western aphasia Bettery-Revised. San Antonio, TX: Pearson, 2006.
18. Kaplan E, Goodglass H, Weintraub S. Boston Naming Test-2. Austin, TX: Pro-Ed, 2001.
19. Howard D, Patterson K. The Pyramids and Palm Trees Test. A test of semantic access from words and pictures. Bury St. Edmunds: Thames Valley Company, 1992.
20. Folstein MF, Folstein SE, McHugh PR. ŌĆ£Mini Mental StateŌĆØ: a practical method for grading the mental status of patients for the clinician. J Psychiatr Res. 1975;12:189ŌĆō198.   23. Goodglass H, Kaplan E, Barresi B. Boston Diagnostic Aphasia Examination. 3rd Ed. Philadelphia, PA: Lippincott Williams & Wilkins, 2001.
24. Nicholas LE, Brookshire RH. A system for quantifying the informativeness and efficiency of the connected speech of adults with aphasia. J Speech Lang Hear Res. 1993;36:338ŌĆō350.  26. Berndt RS, Wayland S, Rochon E, Saffran E, Schwartz M. Quantitative production analysis: A training manual for the analysis of aphasic sentence production. Hove, UK: Psychology Press, 2000.
|
|












